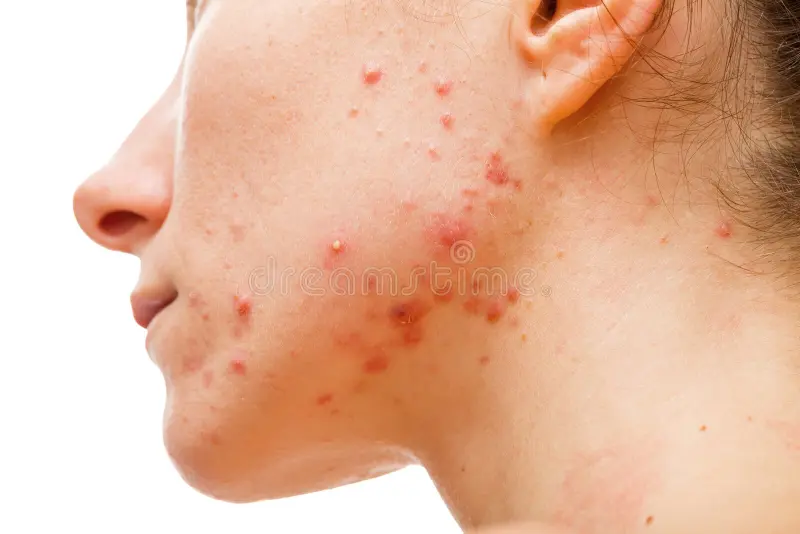
Why Your Acne Keeps Coming Back: Causes & Solutions

Patients ask me this almost every day. Someone comes in after months of trying different face washes, cutting out oily food, following a ten-step routine they found online — and the acne is still there. Sometimes it clears for two or three weeks, then returns in the same spots. Sometimes it shifts location. Sometimes it gets worse right when they thought they had it under control. If you are dealing with acne that keeps coming back, recurring breakouts that no product seems to fix permanently, or persistent hormonal acne that flares every few weeks — this article will give you a clearer picture of what is actually going on and what acne solutions are worth considering.
The Surface Is Not Where the Problem Lives
Most people treat acne as a skin hygiene issue. It is not. The breakout you see on your face is the end result of a process that started much earlier — inside your oil glands, your gut, your bloodstream, or your hormonal system. Cleaning your face more aggressively does not reach any of those places. It only affects the very outermost layer of skin, which is rarely where the real problem is.
This is why so many people cycle through products for years without resolution. They are treating the result, not the cause.
Hormones Are the Most Overlooked Driver
In my clinical experience, hormonal imbalance is behind a significant portion of recurring adult acne cases — particularly in women. Androgens, which are male hormones that both men and women produce, directly stimulate the sebaceous glands to increase oil output. More oil means more congestion in the pores, which creates conditions where acne-causing bacteria multiply faster.
The timing matters. If your breakouts appear predictably around your menstrual cycle — usually on the jawline, chin, or lower cheeks — that pattern is not coincidental. It points to hormonal fluctuation as the trigger. The same applies if you have been diagnosed with PCOS or have irregular periods alongside persistent acne.
No topical product corrects a hormonal imbalance. That requires investigation — blood work, a proper clinical assessment, and sometimes medical management beyond skincare.
Washing More Is Often Making It Worse
This surprises people, but it is one of the more consistent things I observe. Patients who cleanse four or five times a day, layer multiple actives, and aggressively exfoliate are frequently damaging their skin barrier without realising it. A compromised barrier loses moisture faster and triggers the skin to produce more sebum to compensate. That extra sebum feeds the cycle they are trying to break.
The same applies to certain product categories. Alcohol-heavy toners, foaming cleansers that strip everything off, physical scrubs used daily — these are counterproductive for most acne-prone skin types. The skin does not need to be punished. It needs its barrier intact.
Food Connections Are Real, Not Just Anecdotal
There was a period when dermatology largely dismissed diet as a factor in acne. That position has shifted considerably. The evidence around high-glycemic foods is now reasonably solid — refined carbohydrates, sugary drinks, white bread, maida-based foods cause rapid insulin spikes that increase sebum production and promote skin inflammation.
Dairy is more nuanced but worth paying attention to. Milk contains naturally occurring hormones and growth factors that can stimulate oil glands in susceptible individuals. I have had patients who reduced their milk consumption and saw noticeable improvement without changing anything else. Not everyone responds this way, but if your acne has no other clear explanation, diet is worth examining honestly.
Stress Does Not Just Affect Your Mood
Cortisol — the hormone released during stress — increases oil production directly. It also slows the skin’s repair process and aggravates inflammation. The result is more breakouts, slower healing, and more post-acne marks.
What makes this difficult is that acne itself causes stress. The stress worsens the acne. The worsened acne causes more stress. It is a loop that is hard to interrupt without consciously addressing both sides.
I have seen this play out clearly in patients who travel or take extended breaks — skin improves noticeably, then deteriorates again when they return to a high-pressure routine. That is not imagination. That is cortisol.
Long-Term Antibiotic Use Can Stop Working
If you have been on topical or oral antibiotics for acne over an extended period and the results have plateaued or reversed, antibiotic resistance may be a factor. Cutibacterium acnes — the bacterial strain primarily associated with acne — can develop resistance to antibiotics over time, particularly when treatment is inconsistent or prolonged without clinical supervision.
Continuing the same antibiotic in that situation adds little benefit and can disrupt the broader skin microbiome. This is one of the reasons I advise against picking up antibiotic creams from a chemist without a proper consultation. What cleared someone else’s acne may not be appropriate for your skin or your bacterial profile.
Stopping Treatment Too Early Is Extremely Common
Prescription-grade acne treatments — retinoids, azelaic acid, medically supervised protocols — require at minimum eight to twelve weeks before meaningful improvement shows up. Many patients stop at week three or four, either because nothing visible has changed or because there is an initial purging phase that temporarily makes the skin look worse.
They move on to something else, that does not work either, and the pattern repeats. The conclusion they reach is that their acne is untreatable. In most cases, what actually happened is that nothing was continued long enough to work.
What to Actually Do
The starting point is an accurate diagnosis. Acne is not one condition — it is a category. Hormonal acne, fungal acne, comedonal acne, cystic acne, and bacterial acne respond to different treatments entirely. Using the wrong approach not only fails but can sometimes worsen the specific type you have. A clinical assessment gives you a clear direction instead of guesswork.
Internal factors need attention alongside topical ones. If hormones are driving the breakouts, that requires appropriate medical management. If diet is a consistent trigger, it needs to be adjusted. If stress is a significant factor, addressing only the skin while ignoring everything else will produce limited results.
The skin barrier matters more than most people realise. A gentle cleanser, a non-comedogenic moisturiser, and daily SPF are not optional extras. They are foundational to any acne management plan that works over time.
For patients whose acne has not responded to products over a sustained period, clinic-based treatments offer a different level of intervention — chemical peels, targeted extractions, prescription protocols, and in some cases energy-based procedures. At Atomic Clinic, this is typically where patients who have spent years cycling through products finally see lasting results, because we are working at the level where the problem actually originates.
Conclusion
Recurring acne has causes. It is not random, and it is not permanent. But identifying those causes requires looking beyond the surface — at hormones, diet, stress, skincare habits, and treatment history together.
If your acne keeps returning despite consistent effort, the effort may be going in the wrong direction. A proper evaluation changes that. It is where most of my patients who eventually clear their skin actually start.



